The problem
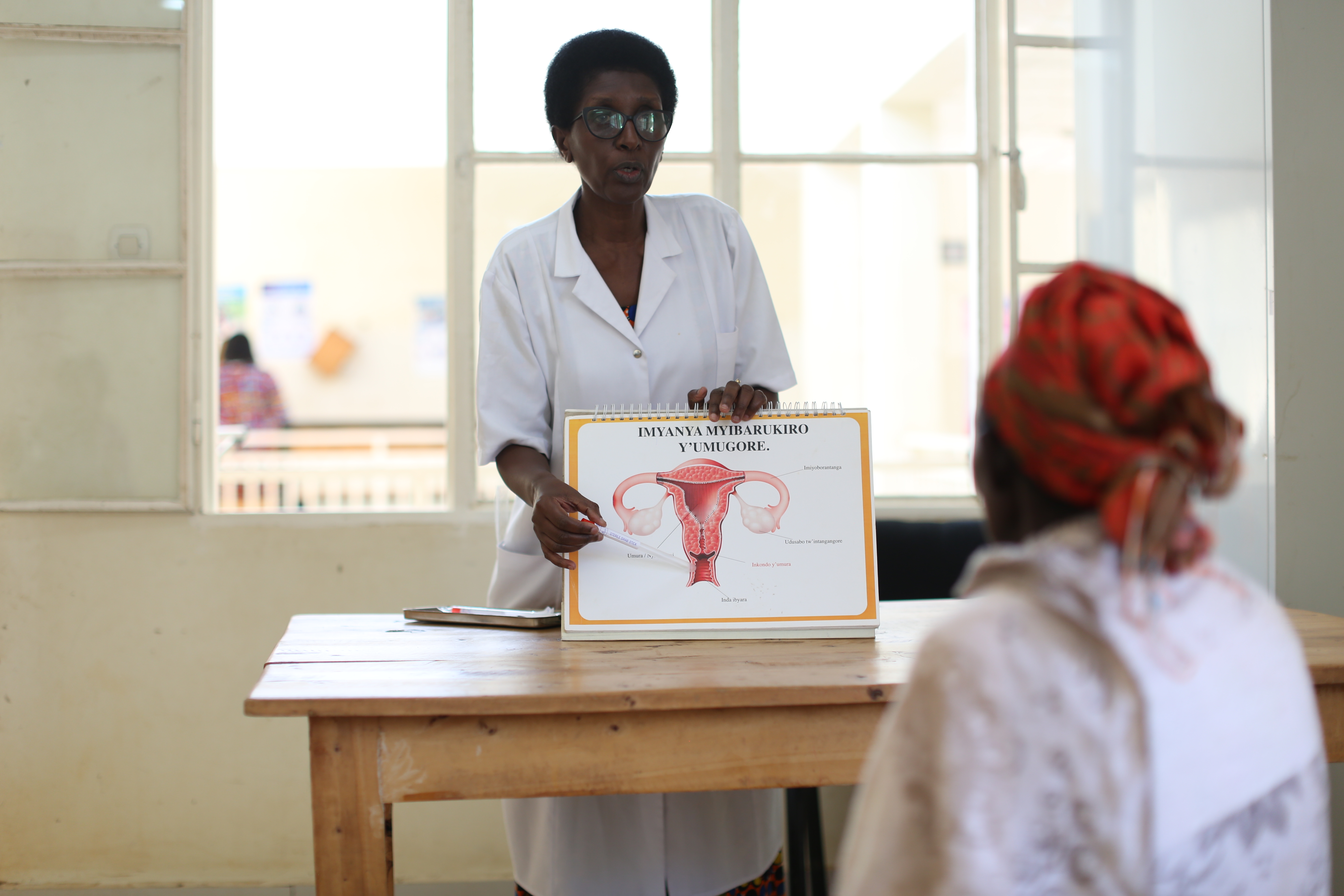
In sub-Saharan Africa where rates of HIV are the highest, new infections are more common among women. Many women learn of their HIV status through routine screening in pregnancy, often in the second or third trimester. Antiretroviral treatments can successfully bring down a woman’s viral load and avert onward transmission to their child at birth, but fast-acting medicines are critical to ensure viral suppression is achieved in time.
In 2016, a new drug called dolutegravir (DTG) had shown to reduce viral load more quickly than the previous efavirenz-based first-line treatment, but it hadn’t been tested in pregnancy, restricting access for many women.
Progress
The DolPHIN2 trial commenced in 2017 in South Africa and Uganda and the findings showed that 74 percent of women receiving DTG achieved viral suppression when giving birth, versus 43 percent in those receiving efavirenz.
In parallel, a qualitative research study that aimed to identify barriers to the implementation of DTG for use in late-presenting pregnant women showed that the transition to DTG-based regimens had the potential to strengthen health systems in low- and middle-income countries and engender equitable access to optimized antiretroviral regimen among women.
Most importantly, data from the trial, along with other studies, informed the revision of the World Health Organization’s HIV treatment guidelines in July 2019 to recommend DTG for all populations as first-line antiretroviral treatment.
Alongside two other Unitaid-funded clinical trials into the use of DTG, this study revealed weight gain and hyperglycemia safety signals that appeared mainly concentrated among African populations. To fully investigate these outcomes, Unitaid approved the TRIO trials, a pooled initiative which permits the extension of three treatment optimization studies; ADVANCE, NAMSAL, and DolPHIN2 to reach 192-week observations. This allows for a longer monitoring period in addition to an opportunity to coordinate and pool data.
COHIVE, a COVID-19 sub-study was included in the three DTG trials to assess the impact of COVID-19 in people living with HIV.