The problem
Despite significant increases in HIV treatment coverage in the years preceding this work, in 2015 more than half (54%) of all people living with HIV still were not on treatment. Many of those people without access were in eastern and southern Africa, the regions most affected by HIV.
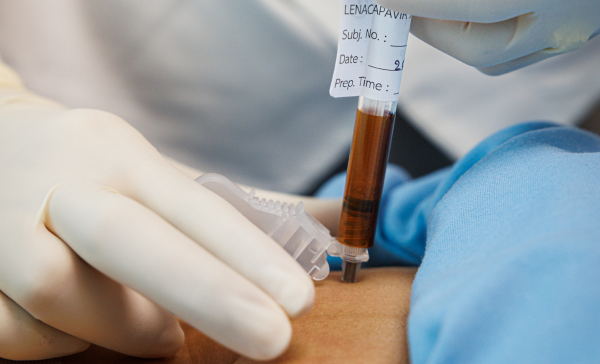
The new antiretroviral drug dolutegravir (DTG) had shown to be simpler and more tolerable for patients, with the potential to improve treatment coverage, but its suitability in resource-limited settings was unknown because it had mainly been evaluated in American and European markets.
Our response
The New Antiretroviral and Monitoring Strategies in HIV-infected Adults in Low-income countries (NAMSAL) trial began in 2016 in Cameroon to investigate the efficacy of DTG-based first-line treatment in a low-income country.
Data from the trial, along with other studies, helped solidify DTG as the first-line treatment in resource-limited settings, contributing to the revision of the World Health Organization’s HIV treatment guidelines in July 2019 to recommend DTG for all populations. It also guided the Cameroonian Ministry of Health to revise its treatment guidelines to include DTG and Efavirenz 400, another HIV life-saving medicine, as first-line protocol.
Alongside two other Unitaid-backed trials, NAMSAL revealed certain side effects of DTG not seen in other populations, highlighting the need to include diverse affected populations in clinical research. Weight gain and hyperglycemia safety signals were associated with dolutegravir in some populations, and the NAMSAL trial was extended to reach 192-week outcomes along with Unitaid-supported ADVANCE and DoLPHIN-2 trials (collectively known as TRIO) to allow for a longer monitoring period in addition to an opportunity to coordinate and pool data.