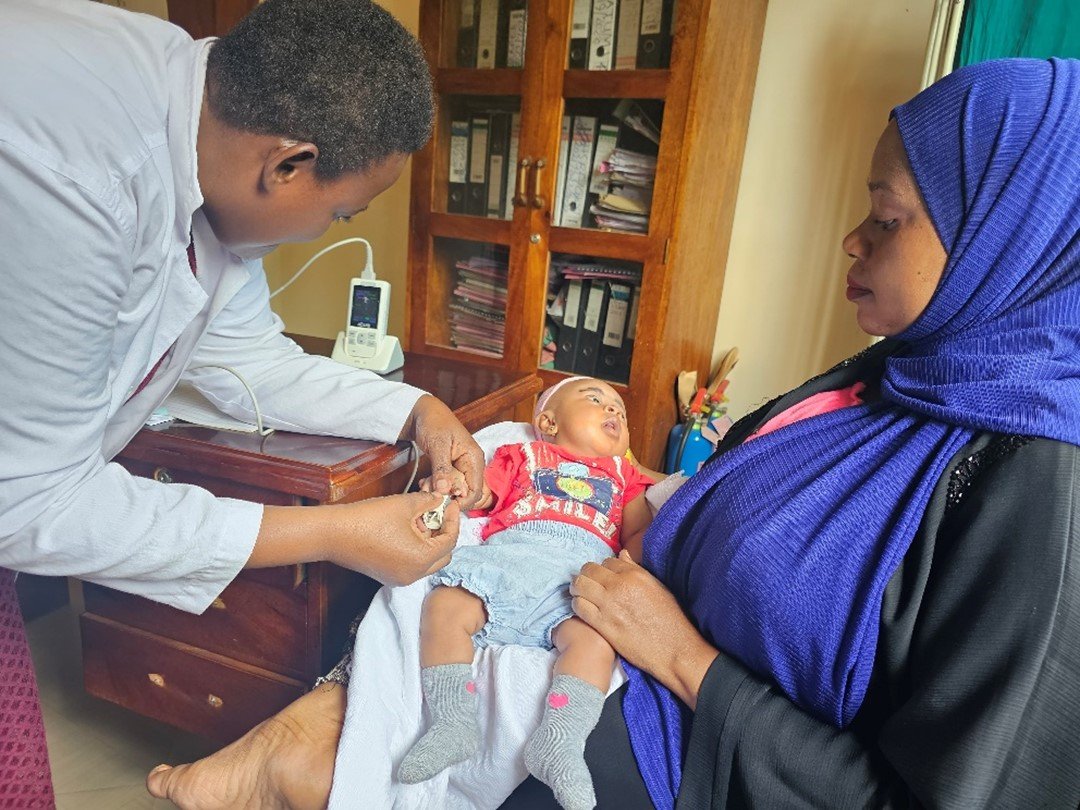
The problem
At the start of this project in 2019, 5.3 million children died before the age of 5, most of them from diseases that can be prevented and treated. Low oxygen in the blood is one of the main signs of severe illness, but devices for measuring oxygen levels, called pulse oximeters, were often not available in lower levels of the health system in lower-income countries, despite being recommended by the World Health Organization. Without standard specifications to guide countries in choosing the best devices, or information on their cost-effectiveness or suitability in primary care, uptake of the devices has been slow.
Download the project evaluation
Our response
This project aimed to equip frontline health care workers with tools to identify severely ill children and provide better care by deploying easy-to-use pulse oximeters in primary health care settings. Working in collaboration with another Unitaid-backed initiative, the TIMCI project, AIRE gathered data on the affordability, feasibility and impact of pulse oximeters, alongside electronic clinical decision support algorithms to improve the quality of care. Across the broader portfolio, all countries reported significant policy progress and commitment towards adopting child-friendly pulse oximeters to enable quicker and more accurate diagnosis of severe disease.