The problem
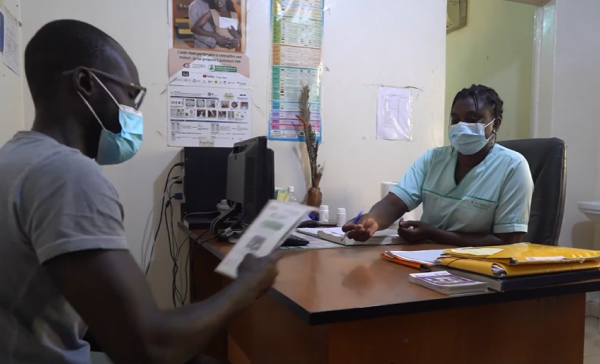
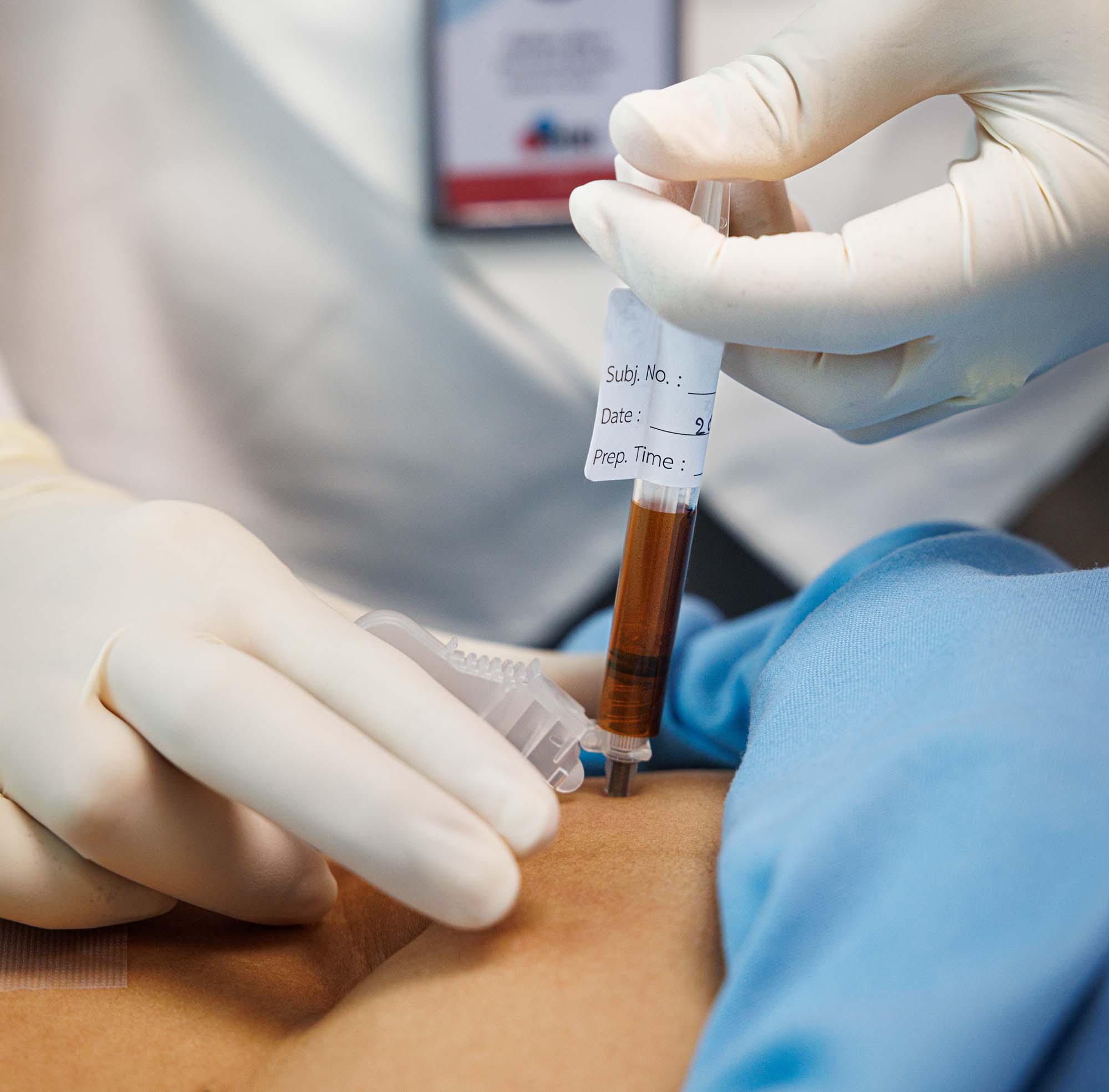
In 2015 when this program began, nearly half (46%) of all people living with HIV worldwide did not know it, which put them at risk of serious illness and of transmitting the virus to others. Testing was only possible within health clinics, and some tests required laboratory processing which could take several days to a week before giving results. Rapid tests were becoming increasingly available but take-home self-tests were not. Many people had concerns about self-testing, doubting the accuracy and reliability of testing if conducted outside health services, as well as fears about how a person might react to getting an HIV-positive result without emotional support services.
Download the project evaluation
Our response
By the time the HIV Self-Testing Africa Initiative (STAR) ended in 2024, 86% of all people living with HIV knew their status and self-testing had become a cornerstone of the HIV response, helping to make important inroads amongst communities that demonstrated lower levels of HIV testing, such as young people, men, and first-time testers.
The STAR project was instrumental in catalyzing the adoption of HIV self-testing strategies across Africa and beyond, with more than 4.8 million self-testing kits distributed, four low-cost blood and saliva-based HIV self-tests pre-qualified by the World Health Organization, and 102 countries with HIV self-testing policies by the project’s end.
Building upon these learnings, Unitaid backed the STAR project to advance similar self-testing approaches for hepatitis C, a common coinfection among people living with HIV. STAR explored the feasibility, acceptability, accuracy, costs and cost-effectiveness of hepatitis C self-testing across various settings.
The STAR project was part of a larger Unitaid-backed effort to advance self-testing. A project led by Solthis in West Africa complemented efforts and contributed to the success of self-testing more broadly.
Self-testing approaches are now being used more broadly in global health as an important way to counter testing hesitancy and help reach more people. Lessons and research from Unitaid’s HIV self-testing efforts have informed approaches for hepatitis C, COVID-19, and the human papillomavirus, an infection that can progress to cervical cancer if left untreated.